
Chronic Pain Clinic
Specialist assessment and wholistic integrated care for persistent and complex pain that hasn't responded to standard treatment — in Greenwich and Canary Wharf, London.
ZENITH OSTEOPATHY + WELLNESS
Persistent Pain is rarely simple…
When pain continues beyond the expected recovery window — or keeps returning despite treatment — it usually means something in the picture hasn't been fully addressed. Not because nothing can be done, but because the assessment hasn't gone far enough.
Standard care is often well-suited to acute injury. For chronic and complex pain, it tends to fall short — not because clinicians don't care, but because the system doesn't allow the time, depth, or integration that these presentations genuinely require.
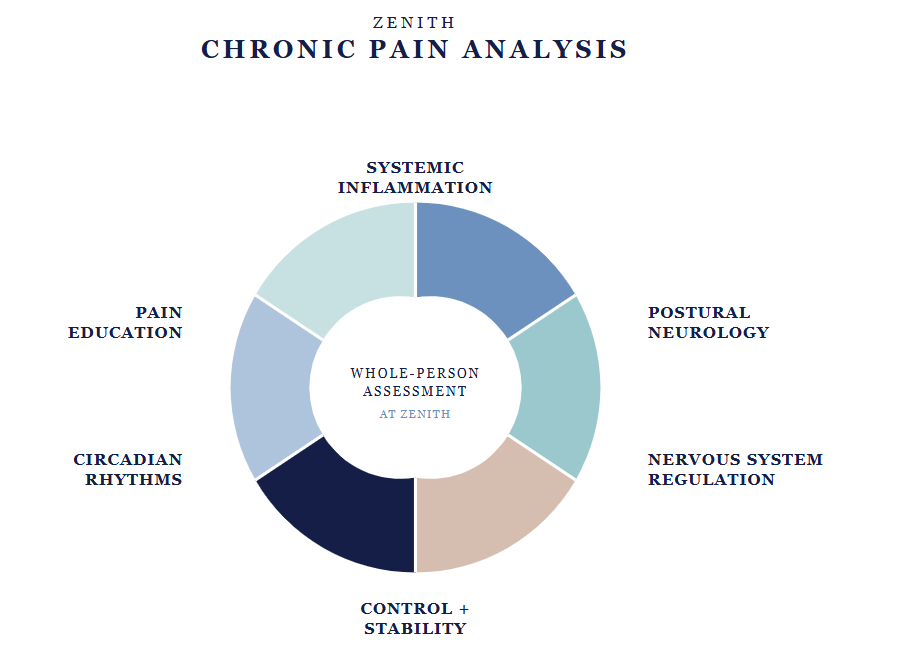
At Zenith, chronic pain is assessed across six interconnected dimensions. Each one can be a driver of persistent pain — and in complex presentations, several are usually involved at once.
-
Chronic inflammation driven by diet, environmental toxins, gut health, and lifestyle can sensitise the nervous system and maintain a pain state long after the original injury has healed. Addressing the inflammatory picture is often a missing piece in complex pain care.
-
How your body holds itself and distributes load over time directly influences which structures are under strain. Postural patterns — often invisible until assessed objectively — are a frequent and underappreciated contributor to persistent pain, particularly in the back, neck, hips, and shoulders.
-
The nervous system is not a passive messenger — it actively modulates pain. Chronic stress, elevated cortisol, and a dysregulated autonomic nervous system can amplify pain signals and slow recovery. Addressing nervous system function directly is often what makes everything else work better.
-
Persistent pain frequently impairs the body's ability to stabilise and control movement — creating compensation patterns that load the wrong structures and perpetuate the problem. Rebuilding strength, proprioception, and neuromuscular control is essential for lasting change, not optional extra rehabilitation.
-
Sleep quality and circadian regulation have a direct, measurable effect on pain perception, tissue repair, and stress hormone balance. Poor sleep doesn't just worsen pain — it actively impairs recovery. It is assessed and addressed as a clinical priority, not an afterthought.
-
Understanding what is driving your pain — and what isn't — changes how you experience it. Evidence consistently shows that pain education reduces fear, improves function, and supports better outcomes. At Zenith, equipping you to understand your own body is part of the treatment, not a supplement to it.

Is this you?
The Chronic & Complex Pain Clinic is for people whose pain has persisted beyond three months — or whose pain keeps returning despite previous treatment. You may recognise yourself in one or more of the following:
Pain that has lasted three months or more, with or without a clear diagnosis
Chronic back or neck pain that hasn't fully resolved with previous care
Pain following an injury that should have healed but hasn't
Pain that seems to move, spread, or show up in multiple places
Hypermobility-related pain — joints that feel unstable, fatigue easily, or cause widespread aching
Pain that worsens during periods of stress, poor sleep, or low mood
A sense that your nervous system is stuck — heightened sensitivity, pain out of proportion to what's happening in the tissue
You don't need a formal diagnosis to book. If pain has become a persistent feature of your life, a thorough assessment is the right starting point.
This clinic is also for people who have been through the system — seen multiple clinicians, tried multiple approaches — and haven't found lasting change. Complex pain often requires a different kind of assessment, not just more of the same treatment.
The Approach
Osteopathy & IASTM
The structural foundation of care. Osteopathic assessment identifies the mechanical contributors to your pain — joint restrictions, soft tissue dysfunction, movement compensations, and postural loading patterns. IASTM (instrument assisted soft tissue mobilisation) is used where fascial restrictions, scar tissue, or chronic tissue changes are part of the picture, working precisely on the layers that manual therapy alone can't fully reach.2. Treat the Root, Not Just the Symptoms
I look beyond the pain to understand what’s causing it.
Poor posture, muscle imbalances, movement patterns, stress, or past injuries can all play a role.
Your treatment plan will address both the immediate pain and the underlying cause.
Medical Acupuncture
One of the most effective tools available for chronic pain modulation. Fine needles placed into targeted points stimulate the body's own pain-relieving mechanisms — reducing nervous system sensitisation, releasing trigger points, and improving the tissue environment. Particularly valuable for presentations where pain has become amplified or where standard hands-on treatment alone hasn't been sufficient.
Vagus Nerve Therapy
For presentations where the nervous system is a significant part of the picture — chronic pain with a strong stress component, pain that flares with emotional load, or a system that feels persistently activated — vagus nerve therapy offers direct support. AVNT (auricular vagus nerve therapy) uses gentle, clinically validated stimulation to support the body's shift from a state of activation and threat toward rest and recovery. Addressing the nervous system environment is often what makes other treatment stick.
Posture Analysis
Where postural loading patterns are contributing to persistent pain — particularly in the back, neck, hips, or shoulders — objective posture analysis provides data that informs both treatment and rehabilitation. Understanding how your body distributes load over time is often a missing piece in chronic pain care.
Health Coaching & Physiological Insights
For presentations where lifestyle, stress, or behavioural patterns are driving or maintaining pain, health coaching brings a clinical understanding of stress physiology and behaviour change into the conversation. Where chronic stress is a significant driver, physiological monitoring is available as an optional add-on — providing objective data on stress load, recovery, and sleep quality to inform the care plan with evidence rather than self-report alone.
Understanding Chronic Pain
Pain is always real. But chronic pain (pain that persists well beyond the expected healing period) isn't always a straightforward signal of ongoing tissue damage. Over time, the nervous system itself can become part of the problem.
When pain persists, the nervous system can become sensitised, meaning it starts to amplify pain signals, respond to stimuli that wouldn't normally cause pain, and maintain a heightened state of alertness that makes recovery harder. This is sometimes called central sensitisation, and it's one of the key reasons chronic pain doesn't always respond to treatment that targets the tissue alone.
This doesn't make the pain less real or less treatable. It means the treatment approach needs to address both the physical drivers (tissue health, joint mechanics, movement patterns) and the nervous system environment in which all of that is happening. At Zenith OW, both are part of every care plan.
Other factors also shape chronic pain presentations and are always considered in assessment: hypermobility and connective tissue vulnerability, the history and mechanics of the original injury, postural loading patterns, sleep quality, and the cumulative effect of stress on the body's capacity to recover
What to Expect
Every clinic at Zenith O+W follows the same careful process: assess first, treat purposefully, and equip you to understand your own body. If you'd like to know more about how care works here before booking, you can read about the approach here.
Your First Appointment
Your initial session is a comprehensive assessment — covering your full case history, a detailed examination of the areas involved, and a clinical picture of what's driving your pain. This includes not just the structural and mechanical picture, but the broader context: your history, your lifestyle, how your nervous system is responding, and what previous treatment has and hasn't addressed.
Treatment begins in this session. You will leave with a clear understanding of what's going on, why it's persisting, and what the plan is. Nothing is done without explanation.
Your Care Plan
Following your initial assessment, a personalised care plan is built around your specific presentation — determining which treatments to use, in what order, and at what frequency. Chronic and complex pain presentations vary significantly in how long they take to resolve. Some people see meaningful change within a handful of sessions; others — particularly those with long-standing sensitisation, hypermobility, or a complex history — will need a longer programme. Your care plan will reflect that honestly from the outset, and will be adjusted as you progress.
Ongoing Review
Your response to treatment is monitored at every session. The plan evolves as you do — because what's needed early in a course of care is rarely what's needed later. The goal is always resolution, or the best achievable function, not indefinite management.
Working Alongside Other Specialists
Complex pain often sits across specialties, and the best outcomes sometimes require a coordinated approach. Where appropriate, Zenith works alongside GPs, pain specialists, rheumatologists, physiotherapists, and other healthcare professionals to ensure your care is joined up rather than fragmented.
If you are already under the care of another clinician or specialist, that context is always factored into your assessment and care plan. And if referral or co-management would benefit your outcomes, we will tell you.
Ready to get a clearer picture of what's driving your pain, and Start Your Recovery?
Book an initial assessment, or get in touch with a question first. If you're not sure whether the Chronic & Complex Pain Clinic is the right fit, a brief conversation is always the best starting point.
